Artificial Intelligence for Neuroplasticity-Based Mental Health Interventions: Detecting and Promoting Adaptive Thought Patterns through Digital Phenotyping
Keywords:
Artificial intelligence, neuroplasticity, digital phenotyping, natural language processing, reinforcement learningAbstract
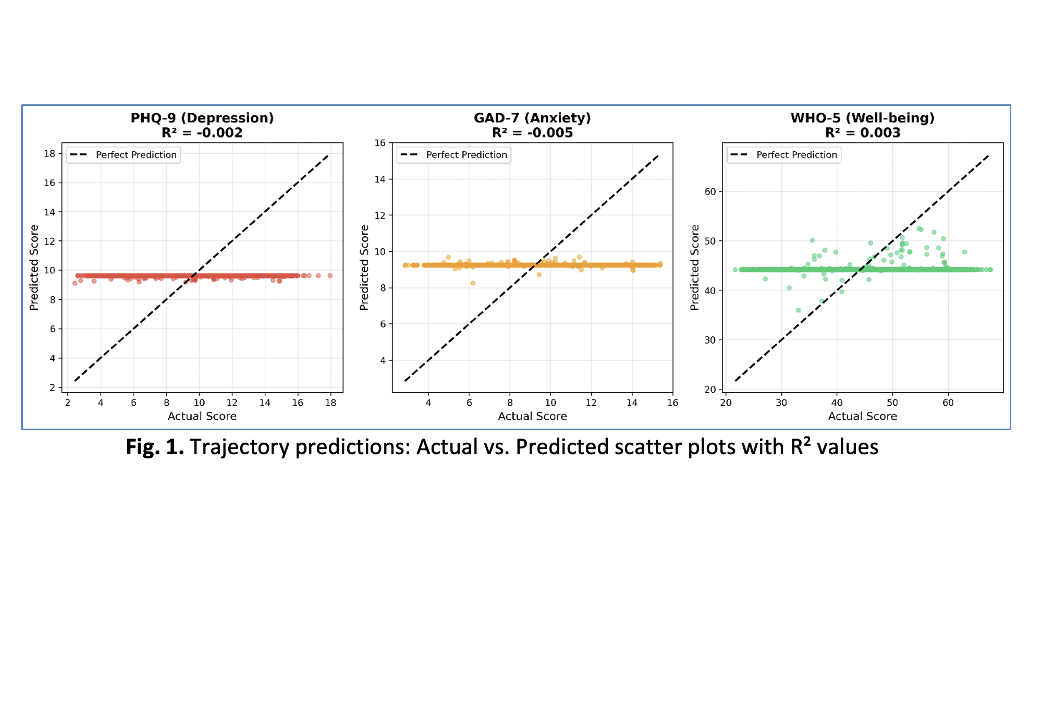
Over 1 billion people experience mental health disorders worldwide, yet conventional approaches struggle with challenges such as scalability, costs, and responsiveness. Neuroplasticity studies indicate that focused cultivation of adaptive patterns of thought such as forgiveness, gratitude, and contentment over 90–180 days are capable of permanently remodeling neural circuits due to improved neurotransmitter modulation and structural brain alterations. This paper presents an AI framework that combines natural language processing (BERT), temporal modeling (LSTM), and reinforcement learning (contextual bandits) to extract and capture the patterns of thought in digital phenotyping data to deliver at scale personalized neuroplasticity-based interventions. The system organizes these in 10 categories (5 adaptive and 5 maladaptive thought patterns), predicts mental health trajectories seven days ahead, and improves delivery by learning from policies. Technical feasibility proof of concept with 500 synthetic participants, 12 weeks: NLP classification achieved 87% accuracy, and thought patterns predicted depression (r = ±0.30) and reinforcement learning prioritizing appropriate interventions was effectively used for them (gratitude prompts: 44.5% selection rate, 0.60 reward), showing that we could pull off proof of concept implementation. Full AI intervention group exhibited +24% more adaptive pattern improvements and -21% less maladaptive changes by 90 days, indicating clear neuroplastic change of patterns from maladaptive-dominant to adaptive-dominant thinking. Nevertheless, there were only slight differences in clinical results (PHQ-9: -0.2 points), therefore indicating the incongruence between mechanism engagement and symptom reduction within this synthetic data. Through operationalizing the 90–180-day window for neuroplastic consolidation using milestone tracking, the model delivers cost-effective, scalable mental health support that empowers individuals to purposefully guide their neural configurations. It is a departure from static, reactive symptom management to proactive neural circuit adaptation through self-directed neuroplasticity rooted in neuroscience, positive psychology, and theological anthropology. Strong clinical validation via randomized controlled trials is still necessary to obtain real-life efficacy, with a focus on equity, culture, and ethics in practice.